Corneal Transplantation.
East Valley Ophthalmology in Mesa, Arizona specializes in state-of-the-art
corneal transplantation. Corneal transplantation, also known as
corneal grafting or penetrating keratoplasty (PKP), is a surgical
procedure where a damaged cornea is replaced by donated corneal
tissue. For information beyond what is available on our website,
please call: 480-981-6111.
Penetrating Keratoplasty (PKP)
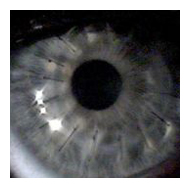 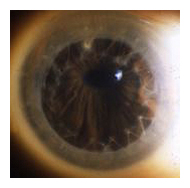
Penetrating keratoplasty (PKP) is full-thickness
corneal transplant. It was first developed over 100 years ago
and is now one of the most common transplant procedures. Although
approximately 100,000 procedures are performed worldwide each
year, some estimates report that 10,000,000 people are affected
by various disorders that would benefit from corneal transplantation.
In the United States, the cost is usually covered in part by Medicare
and health insurers. Reimbursement depends on your personal healthcare
provider.
Also see Partial-Thickness Corneal Transplant:
DSEK (Descemet's
Stripping Endothelial Keratoplasty)
Indications
A corneal transplant is done for a variety of conditions that
lead to poor vision. These include Fuchs' corneal dystrophy, bullous
keratopathy, herpes keratitis, and sometimes ocular trauma. Indications
for corneal transplantation include the following:
- Optical: To improve visual acuity by replacing
the opaque host tissue by clear healthy donor tissue. The most
common indication in this category is pseudophakic bullous keratopathy,
followed by keratoconus, corneal degeneration, keratoglobus and
dystrophy, as well as scarring due to keratitis and trauma.
- Tectonic/reconstructive: To preserve corneal anatomy and
integrity in patients with stromal thinning and descemetoceles, or to reconstruct
the anatomy of the eye, e.g. after corneal perforation.
- Therapeutic: To remove inflamed corneal tissue unresponsive
to treatment by antibiotics or anti-virals.
- Cosmetic: To improve the appearance of patients with corneal
scars that have given a whitish or opaque hue to the cornea.
Pre-operative Examination
At East Valley Ophthalmology, you will meet with your
ophthalmologist for an examination in the weeks or months preceding
your surgery. The doctor will examine your eye, make a diagnosis
and, if indicated, order lab tests, such as blood work, X-rays,
or an EKG. He will discuss the condition of your eye with you
and the available treatments, including the
risks and benefits of each. Your surgery date and time will
be set, and you will sign a consent form and be told where
the surgery will take place.
Procedure of Corneal Transplantation
On the day of the surgery, you will arrive to the outpatient
surgery center, where the procedure will be performed. You will
be given a brief physical examination by the surgical team and
is taken to the operating room. In the OR, you will lie down
on an operating table and either given general anesthesia,
or local anesthesia and a sedative.
With anesthesia induced, the surgical team prepares the eye to
be operated on and drapes the face around the eye. An eyelid speculum
is placed to keep the lids open, and some lubrication is placed
on the eye to prevent drying. A metal ring is then stitched to
the sclera, which will provide a base for a trephine.
A trephine is then placed over the cornea and is used by the
surgeon to cut the host cornea. The trephine is then removed and
the surgeon cuts a circular graft (a "button") from
the donor cornea. Once this is done, the surgeon returns to the
eye and removes the host cornea.
The donor cornea is then brought into the surgical field and
maneuvered into place with forceps. Once in place, the surgeon
will fasten the cornea to the eye. The surgeon finishes up by
reforming the anterior chamber with a sterile solution injected
by a canula, then testing that it's watertight by placing a dye
on the wound exterior.
With the metal ring removed and antibiotic eyedrops placed, the
eye is patched, and you will be taken to a recovery area while
the effects of the anesthesia wear off. You may
go home following this and see the doctor the following day
for your first post-operative appointment.
Prognosis of Corneal Transplantation
When the primary
purpose of a cornea transplant is to improve visual acuity, the
prognosis is dependent upon whether the rest of the eye is healthy.
If it is, then it should be possible to recover normal vision.
Full visual recovery can take 6 to 12 months.
Risks of Corneal Transplantation
Traditional corneal transplant surgery has about a 90% success
rate, and the rate of rejection is only about 8%. Rejection episodes
can often be controlled with topical steroid drops. Graft failure
can occur at any time after the cornea has been transplanted,
even years or decades later. The causes can vary, though it is
usually due to new injury or illness. Treatment can be either
medical or surgical, depending on the individual case.
Occasionally,
there are problems with sutures, which can come loose, cause infections,
or cause astigmatism. The astigmatism after traditional corneal
transplant surgery can be significant enough that eyeglasses alone
won't give adequate vision. These patients may ultimately
require contact lenses or additional surgery to reduce or eliminate
the astigmatism.
Because the wound is full-thickenss and 360 degrees,
the corneal transplant wound is not as strong as normal. It is
at risk to rupture or break open from mild or incidental trauma,
even several years after the surgery.
While the cornea is avascular, there is still a potential for
some blood loss, usually from suturing the metal ring to the sclera.
Any blood loss is typically less than a teaspoon, or less than
2 cc.
There is also a risk of infection. Since the cornea has no blood
vessels (it takes its nutrients from the aqueous humor) it heals
much slower than a cut on the skin. While the wound is healing,
it is possible that it might become infected by various microorganisms.
This risk is minimized by antibiotic prophylaxis (using antibiotic
eyedrops, even when no infection exists).
The eye specialists of East Valley Ophthalmology perform advanced
technology diagnostic testing and treatment, as well as taking
the time necessary to provide each patient with information needed
to fully understand their condition and to achieve their best possible
visual outcome.
If you would like further information, please call our office at:
480-981-6111
East Valley Ophthalmology
Eye Doctors - Mesa, ArizonaIf you or a family member
or friend have not had a recent routine eye examination, have a specific eye condition that needs addressing, or are looking for
an eye specialist or professional eye consultant please take a moment to Request an Appointment.
|