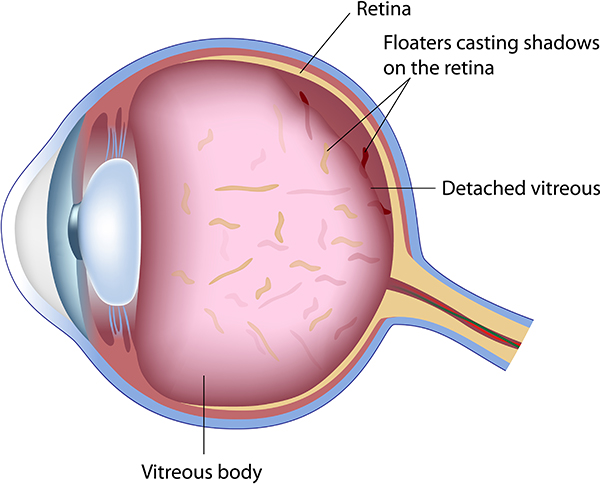
The most common cause of floaters and flashes is posterior vitreous detachment (PVD), a prevalent eye condition. PVD is caused by natural changes to the transparent fluid-gel (vitreous) that takes up the space inside the eye. As a regular part of aging, the vitreous can shrink and pull away from the retina. PVD doesn’t cause pain, harm the eye, or cause permanent vision loss. PVD happens typically over a period of time, and it’s something that you won’t feel happening.
Flashes & Floaters
 Floaters are deposits of various sizes, shapes, and consistencies, floating within the vitreous. These may appear as spots, threads, or fragments of cobwebs, singly or together with several others in one’s field of vision. They are especially noticeable when looking at a blank surface or an open monochromal space, such as a clear blue sky.
Floaters are deposits of various sizes, shapes, and consistencies, floating within the vitreous. These may appear as spots, threads, or fragments of cobwebs, singly or together with several others in one’s field of vision. They are especially noticeable when looking at a blank surface or an open monochromal space, such as a clear blue sky.
Despite the name “floaters”, many of these specks tend to sink toward the bottom of the eyeball in whichever way the eyeball is oriented. Looking up or lying back tends to concentrate them near the center of one’s gaze. A textureless and evenly lit sky forms an ideal background against which to view them.
Sometimes fine dark lines, like small branching twigs in an amorphous mass, are seen. These floaters move around and are called ‘muscae volitantes’ (Latin for ‘flying flies’), because they seem to dart about like flies as the eye is moved. Over time, you will become less aware of these floaters as the brain learns to ignore them. And that is why, while some floaters may remain in your vision, many of them appear to fade over time and become less bothersome.
Floaters are common and do not cause problems for most people. In fact, given some time, people usually learn to ignore them. However, for some people with severe cases, floaters can be a significant distraction — especially if the spots appear to drift constantly through the field of vision.
Floaters have been known to catch and refract light in ways that somewhat blur vision temporarily until the floater moves to a different area. Many times, they trick the sufferer into thinking they see something out of the corner of their eye that really is not there. For people with severe floaters, it is nearly impossible to completely ignore the large masses that constantly stay within almost direct view. Some individuals have reported a decrease in their ability to concentrate while reading, watching television, walking outdoors, and driving, especially when they are tired.
Although more common in older adults, floaters can undoubtedly become a problem for younger individuals, especially those with myopia. Floaters are also common after cataract operations or after trauma. In some cases, floaters are present from birth.
The vitreous is a usually clear, gel-like substance that fills the center of the eye. It makes up approximately 2/3 of the eye’s volume, giving it form and shape. Floaters are tiny structures of protein or other cell debris that have accumulated over the years and become trapped inside the vitreous. The shapes that you see are actually shadows projected onto the retina by the floaters. Floaters can even be seen when the eyes are closed, especially on especially bright days, when sufficient light penetrates the eyelids to cast shadows.
Floaters generally follow the rapid motions of the eye, while drifting slowly within the fluid. When they are first noticed, the natural reaction is to attempt to look directly at them. However, trying to shift one’s gaze toward them can be difficult since floaters follow the motion of the eye, remaining to the side of the direction of gaze. In fact, floaters are visible only because they do not remain perfectly fixed within the eye.
Normal blood vessels in the eye also obstruct light, but they are invisible under normal circumstances because they are in a fixed location relative to the retina. The brain ignores stabilized images due to neural adaptation. This does not occur with floaters because they move around and remain visible.
There are other causes for the appearance of floaters, of which the most common are described here. Basically, any way by which material enters the vitreous is a cause for floaters.
What is vitreous syneresis?
The most common cause of floaters is vitreous syneresis – shrinkage of the vitreous.
 In the young eye, the vitreous gel is solid, and the posterior vitreous surface is well attached to the retinal surface. |
 In the aging eye, small pockets of liquefied vitreous (lacunae) can develop within the gel. |
|
 Lacunae may form pockets and lead to separation from the retinal surface. |
 Contraction of the vitreous can produce light flashes or cause physical tears. |
Posterior vitreous detachments and retinal detachments
Over time, as we age, the vitreous loses support and its framework contracts. This may lead to vitreous detachment, in which the vitreous body is released from the retina. During this detachment, the shrinking vitreous can mechanically stimulate the retina, causing the patient to see random flashes across the visual field, sometimes referred to as “flashers.” The ultimate release of the vitreous sometimes makes a large floater appear, usually in the shape of a ring (“Weiss ring”). As a complication, part of the retina might be torn off by the departing vitreous body, in a process known as retinal detachment. This often causes blood to leak into the vitreous, which the patient perceives as a sudden appearance of numerous small dots moving across the entire field of vision.
Regression of the hyaloid artery during pregnancy
The hyaloid artery, an artery running through the vitreous during the fetal stage of development, regresses in the third trimester of pregnancy. Its disintegration can sometimes leave cell matter.
Other common causes
Patients with retinal tears may experience floaters if red blood cells are released from leaky blood vessels, and those with a posterior uveitis or vitritis, as in toxoplasmosis, may experience multiple floaters and decreased vision due to the accumulation of white blood cells in the vitreous humour.
Other causes for floaters include cystoid macular edema and asteroid hyalosis. The latter is an anomaly of the vitreous humour, whereby calcium clumps attach themselves to the collagen network. The bodies formed in this way move slightly with eye movement but then return to their fixed position.
 Sometimes, the appearance of floaters can be attributed to dark specks in the tear film of the eye. Technically, these are not floaters, but they appear the same from the patient’s viewpoint. People with blepharitis or a dysfunctional meibomian gland are especially prone to this condition, but ocular allergies or even the wearing of contact lenses can cause the problem. To differentiate between material in the vitreous of the eye and debris in the tear film, one can look at the effect of blinking: debris in the tear film will move quickly with a blink. At the same time, floaters are unresponsive primarily to it. Tear film debris is diagnosed by eliminating the possibility of floaters and macular degeneration.
Sometimes, the appearance of floaters can be attributed to dark specks in the tear film of the eye. Technically, these are not floaters, but they appear the same from the patient’s viewpoint. People with blepharitis or a dysfunctional meibomian gland are especially prone to this condition, but ocular allergies or even the wearing of contact lenses can cause the problem. To differentiate between material in the vitreous of the eye and debris in the tear film, one can look at the effect of blinking: debris in the tear film will move quickly with a blink. At the same time, floaters are unresponsive primarily to it. Tear film debris is diagnosed by eliminating the possibility of floaters and macular degeneration.
Flashes of light that you see in your field of vision can look like pinpricks or spots, jagged lines, or appear wavy. They may look like shooting stars or lightning streaks.
Flashes occur inside your eye or brain. They are not caused by anything else outside your body. They are usually noticed at night. Flashes lasting a few seconds may result from the vitreous gel inside the eye shrinking or changes, pulling on the retina. This may occur as a natural result of aging or may happen temporarily, such as after receiving a blow to the head or eye.
It is common for people to see occasional flashes of light as they age. Although these flashes are usually harmless, you should discuss them with your ophthalmologist during an eye exam. However, the onset of new light flashes of short duration at night, especially when accompanied by the appearance of many new floaters or a blackening out of part of your field of vision, may indicate a retinal tear or detachment. This is a severe condition that your ophthalmologist must treat quickly to prevent blindness. Call your doctor right away if this happens.
Migraine headaches
Light flashes appearing as wavy lines in both eyes and lasting from a few minutes to half an hour are usually a sign of an ocular migraine headache. Migraine-related flashes are often noticed in a lighted environment. Flashes of this nature are not a symptom of eye problems.
Usually, the appearance of new floaters or light flashes does not indicate any serious eye problem. However, the only way to ensure that the floaters or flashes are not symptomatic of a more serious problem is to have your retina examined. If, after the exam, you develop a large number of new floaters that seem to worsen over time, we recommend that you have your eyes re-examined.
Standard vision tests, such as the Snellen visual acuity measurement, which measures your vision as 20/20, etc., are unable to quantify floaters and how the disability interferes with day-to-day functioning and overall quality of life. Floaters are often readily observed using an ophthalmoscope or slit lamp. However, if the floater is a small piece of debris and near the retina, your eye doctor may not be able to observe it even if it appears large and obvious to you.
Increasing background illumination or using a pinhole to decrease pupil diameter effectively may enable a person to obtain a clearer view of their own floaters. The head may be tilted in such a way that one of the floaters drifts towards the central axis of the eye. In the sharpened image, the fibrous elements are more conspicuous. (If the pinhole is kept moving slowly in small circles, the same technique evokes an interesting entoptic effect known as the vascular figure, which is a view of the blood vessels within one’s own eye.)
For a minor annoyance, when floaters appear in your line of vision, move your eye around — up and down as well as from side to side. This movement creates a swirling in the vitreous fluid and may cause the floater to move out of your field of vision.
In some patients, floaters can cause persistent, distracting, and disabling symptoms. In these patients, visual tasks such as reading or driving become laborious, and productivity and overall quality of life may suffer. It is advisable to wait at least one year to allow enough time for your brain to adjust and the floaters to become less prominent naturally. If they do not, then one may consider vitrectomy surgery or laser surgery as an alternative. We must caution at the very outset of this discussion that laser or surgical treatment of floaters is not considered a standard management strategy and is recommended by a minority of physicians, even then, only under exceptional circumstances.
We are not aware of any vitamins or drugs that can reduce floaters.
Comprehensive eye exams
To safeguard your vision, individuals over age 40 should undergo a comprehensive eye exam annually. Suppose you are under age 40 and have risk factors such as high blood pressure, diabetes, or a family history of glaucoma or macular degeneration. In that case, a yearly exam is also highly recommended. Individuals under the age of 40 who are in good health, with no known risk factors, should have their eyes examined every two years.
Pars plana vitrectomy (PPV)
Pars plana vitrectomy is a procedure usually reserved for complicated posterior segment disease. It has a well-known risk profile, and justifiably, there is reluctance to offer this surgery to treat floaters. However, the postoperative complication rate following PPV has been assessed in the setting of retinal detachment surgery or in the presence of complicated vitreo-retinal disease. It may be argued that pars plana vitrectomy for floaters, in eyes that have an established posterior vitreous detachment, may be associated with a lower incidence of both intraoperative and postoperative complications.
The three main postoperative complications to consider in vitrectomy are the development or progression of nuclear sclerosis cataract, retinal detachment, and choroidal or vitreous hemorrhage (bleeding) in the eye.