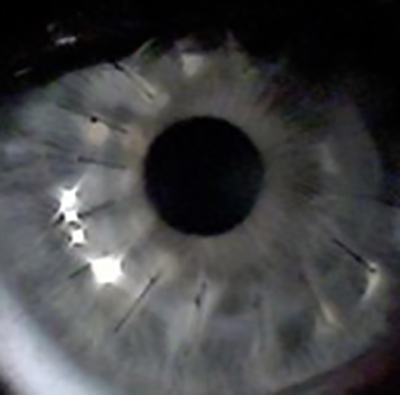
What is corneal transplantation?
If your cornea is damaged and cannot be healed or repaired, your ophthalmologist may recommend a corneal transplant, also known as corneal grafting or penetrating keratoplasty (PKP). This procedure replaces a diseased cornea with a clear, healthy cornea from a human organ donor.
Human donors are individuals who choose to donate their corneas after death to those in need. All donated corneas are thoroughly tested to ensure they are healthy and safe for use.
There are different types of corneal transplants. In some cases, only the front and middle layers of the cornea are replaced (DSEK). In others, only the inner layer is removed (DMEK). Sometimes, the entire cornea needs to be replaced (penetrating keratoplasty, or PKP).
What is penetrating keratoplasty (PKP)?
Penetrating keratoplasty (PKP) is the most common, traditional form of corneal transplantation. PKP is a full-thickness corneal transplant. It was first developed over 100 years ago. Although over 100,000 PKP procedures are performed worldwide each year, some estimates report that there may be 10 million people affected by various disorders that would benefit from corneal transplantation.
In the United States, the cost is usually covered in whole or in part by Medicare and health insurance. Reimbursement depends on your individual healthcare provider.